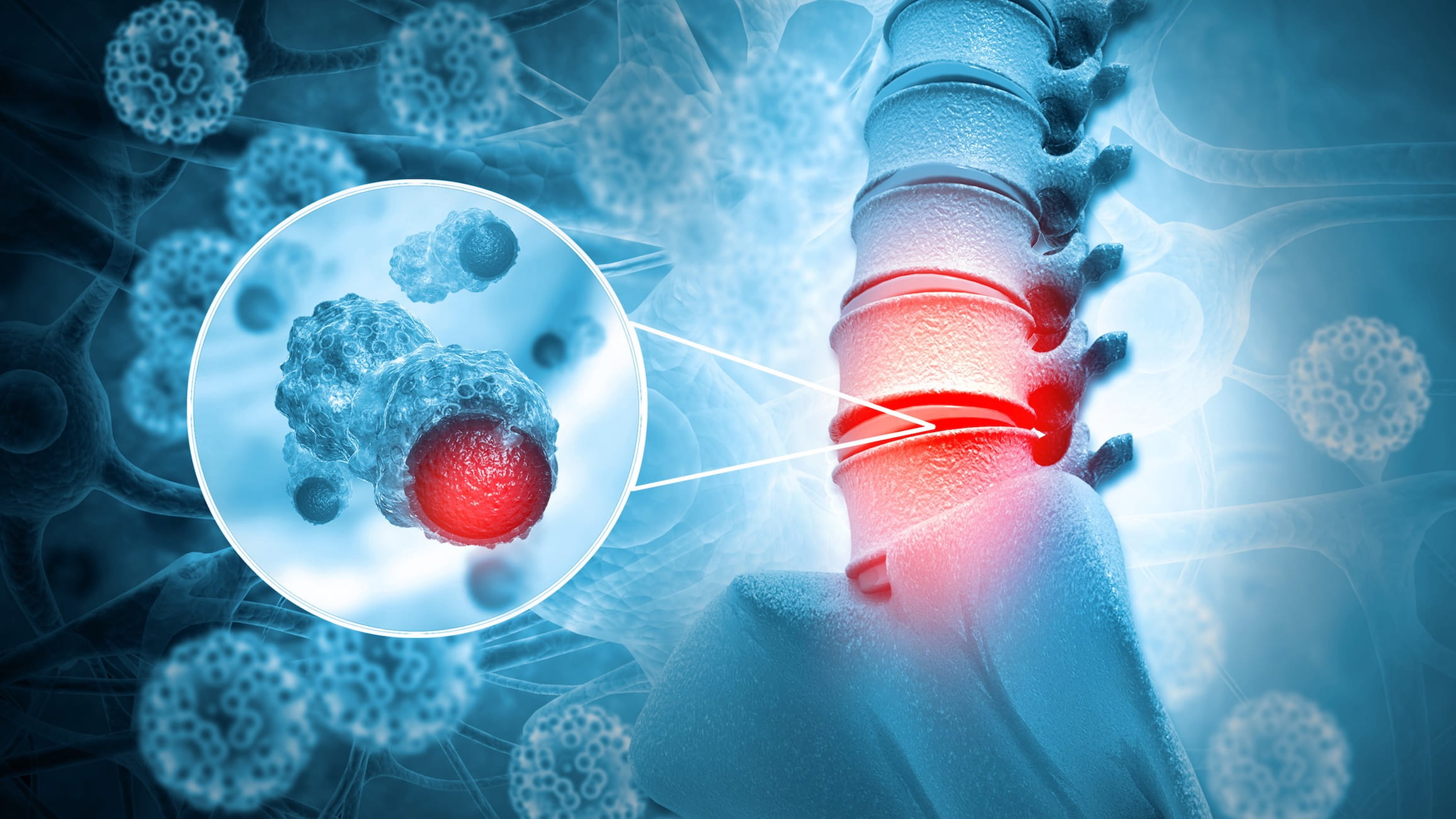
Minimally Invasive Spinal Tumour Surgery: Benefits & Recovery
A spinal tumour diagnosis raises understandable concerns about surgery, recovery and long-term outcomes. Many patients associate spinal procedures with large incisions and prolonged rehabilitation. However, advances in minimally invasive spinal tumour surgery now allow selected tumours to be treated using smaller, tissue-sparing techniques.
This surgical approach focuses on accessing the tumour through targeted pathways. The goal is to remove abnormal tissue while minimising disruption to surrounding muscles, nerves and stabilising structures. For suitable patients, this may lead to reduced postoperative discomfort and a smoother spine tumour surgery recovery experience.
What Is Minimally Invasive Spinal Tumour Surgery
Minimally invasive spine tumour surgery refers to techniques that remove spinal tumours through small incisions using specialised surgical instruments. These procedures are performed with the aid of high-magnification microscopes or endoscopic systems that allow precise visualisation of delicate spinal structures.
Minimally invasive approaches aim to preserve normal tissues. By reducing muscle trauma, the body’s natural healing response may be more efficient, contributing to faster functional recovery in appropriately selected cases.
Key characteristics include:
- Small, precise incisions
- Use of microscopes or endoscopes
- Reduced muscle disruption
- Focused tumour localisation
- Less structural trauma compared with open surgery
When Is Minimally Invasive Surgery Recommended for Spinal Tumours
The suitability of spinal tumour minimally invasive surgery depends on several clinical factors.
Common considerations include:
- Tumour size
- Tumour location within the spine
- Benign vs malignant nature
- Degree of spinal cord or nerve compression
- Patient’s overall health status
Patient-specific considerations are equally important. Overall health status, bone quality, and neurological function influence surgical decision-making. Careful evaluation helps determine whether minimally invasive spine surgery for tumour treatment is appropriate.
When Is Minimally Invasive Surgery Recommended for Spinal Tumours
One of the primary benefits of minimally invasive spine surgery is reduced tissue disruption. Smaller incisions and targeted access pathways may result in less postoperative pain and improved early mobility.
Patients often experience less muscle-related discomfort. Reduced blood loss, shorter operating times in selected cases, and a shorter spinal tumour surgery hospital stay are also commonly associated with minimally invasive techniques.
Importantly, these benefits are closely linked to patient selection. Outcomes depend on tumour characteristics, surgical complexity and overall spinal stability.
Common Pinched Nerve Symptoms

- Factor: Incision Size
- Benefits: Small, targeted incisions

- Factor: Muscle Disruption
- Benefits: Reduced soft tissue impact

- Factor: Postoperative Pain
- Benefits: Less discomfort

- Factor: Hospital Stay
- Benefits: Often shorter duration
- Factor: Recovery Pattern
- Benefits: Typically faster in selected cases
While minimally invasive surgery may offer advantages, open surgery remains essential for complex tumours requiring extensive visualisation or reconstruction.
What Happens During the Procedure
Minimally invasive spine tumour removal follows a structured surgical process. After the patient is placed under general anaesthesia, a small incision is created over the targeted spinal level.
Imaging tools are used to accurately identify the tumour’s location. Specialised instruments are then used to remove tumour tissue while preserving surrounding structures. High-magnification visualisation allows the surgeon to work within narrow spinal spaces safely.
Once tumour removal is completed, the incision is carefully closed. The emphasis throughout the procedure is precision and tissue preservation.
Recovery After Minimally Invasive Spinal Tumour Surgery
Recovery after spinal tumour removal varies depending on tumour type and neurological involvement. However, many patients benefit from earlier mobilisation.
Walking often begins within the early postoperative period, depending on the patient’s neurological status. Pain is managed using a combination of medications.
The overall spinal tumour surgery recovery time is influenced by surgical complexity, spinal stability and the need for rehabilitation. Some patients resume light activities within weeks, while others require longer periods of conditioning.
General Recovery Timeline
First 24–48 Hours
- Patients rest and recover under medical supervision
- Discomfort is managed with appropriate medication
- Gentle assisted movement may begin
Day 3–7
- Surgical soreness typically continues to improve
- Light daily activities are gradually resumed
- Strenuous movements and heavy lifting are avoided
Week 1–4
-
Mobility and comfort usually improve steadily
-
Patients often regain confidence with movement
-
Simple rehabilitation exercises may be introduced
Week 4–8
-
Strength and endurance continue to recover
-
Daily activities become more manageable
-
Gradual return to normal routines may be possible
Week 9–12
-
Most patients tolerate regular activities more easily
-
Functional recovery continues to stabilise
-
Follow-up assessment may be performed if needed
Risks and Possible Complications
As with all procedures, the risks of spine tumour surgery must be discussed. Potential complications include infection, bleeding, nerve irritation, cerebrospinal fluid leaks and tumour recurrence.
Minimally invasive techniques do not eliminate risk but aim to reduce tissue-related complications. Careful surgical planning remains critical.
Success Rate and Long-Term Outcomes
The minimally invasive spine surgery success rate is favourable in carefully selected patients. Surgical outcomes depend on multiple clinical factors, including tumour characteristics and neurological involvement.
Key factors influencing outcomes include:
- Tumour type, size and location
- Degree of nerve or spinal cord compression
- Surgical accessibility
- Preservation of neurological structures
- Postoperative rehabilitation and recovery
Minimally invasive techniques are designed to reduce tissue disruption while allowing effective tumour removal. Long-term follow-up remains essential to monitor spinal stability, assess neurological recovery and detect tumour recurrence where applicable.
When to See Our Spine Surgeon
Patients should seek medical review if they experience:
- Persistent spinal pain that does not improve
- Progressive numbness or tingling
- Muscle weakness in the arms or legs
- Changes in coordination or balance
- A confirmed spinal tumour diagnosis
Early consultation supports accurate diagnosis through clinical assessment and imaging, where needed. Timely intervention planning may reduce the risk of long-term neurological complications.
Frequently Asked Questions
-
When is minimally invasive spinal tumour surgery recommended?
It is considered when the tumour is well-localised and accessible. Our spinal tumour surgeon in Singapore will assess suitability based on tumour size, location and spinal stability. -
How long does minimally invasive spine tumour surgery take?
Surgical duration varies based on tumour complexity and location. Your specialist will provide an estimate during the consultation. -
Is minimally invasive spine surgery safe for tumours?
Safety depends on tumour characteristics and patient suitability. Careful surgical planning is essential. -
What is recovery like after spinal tumour surgery?
Recovery varies between individuals. Many patients begin gentle movement early under medical guidance. -
Can spinal tumours be removed without open surgery?
Some tumours are suitable for minimally invasive spine tumour removal techniques. The decision is case-dependent. -
How painful is minimally invasive spine surgery?
Postoperative discomfort is expected but manageable. Pain control strategies are provided after surgery. -
How soon is walking after spinal tumour surgery possible?
Walking often begins early when clinically appropriate. Timing depends on neurological status and surgical factors. -
How is the cost of spine tumour surgery in Singapore determined?
Costs vary depending on tumour complexity, surgical technique, hospital requirements and postoperative care. Our clinic can provide an individualised estimate after evaluation.
Spine Tumour Surgery at Orthospine Works
At Orthospine Works, patients consulting Dr Gamaliel Tan undergo a detailed evaluation to determine the appropriate treatment strategy. Dr Tan assesses tumour characteristics, spinal stability and neurological involvement before recommending surgical options.
Where clinically suitable, minimally invasive spinal tumour surgery in Singapore may be considered to reduce tissue disruption and support recovery. Treatment planning is individualised, with a focus on safety, functional preservation and long-term spinal health.
Patients receive structured guidance before and after surgery, ensuring clarity throughout the care journey.
If you have been diagnosed with a spinal tumour or are experiencing concerning neurological symptoms, early specialist evaluation is recommended.